More asthma patients achieve the optimal inspiratory flow for high-resistance inhalers than for low-resistance inhalers
Insights | 21/01/2021
Prescribing information and adverse event reporting can be found at the bottom of this page.
- For successful management of asthma, estimating a patient’s peak inspiratory flow rate (PIFR) can help in choosing the most compatible inhaler type.
- In a recent study (Haughney et al, 2020), nearly all patients achieved a PIFR sufficient for high resistance inhalers (DPIs) whereas only two out of three patients were able to generate a PIFR correct for low resistance inhalers (pMDIs).
- All patients who failed the low resistance test inhaled too quickly, including one fifth of patients currently using a pMDI.
Correct inhaler technique is essential for successful drug deposition into the respiratory system. Estimating a patient’s peak inspiratory flow rate (PIFR) can help to select the most suitable inhaler type for the patient’s inhalation abilities, as the optimal PIFR varies based on the device mechanism.
A study by Haughney et al. determined the proportion of patients with asthma capable of producing the correct PIFR for low and high resistance inhalers.
The PIFRs of adult patients were measured with the In-Check DIAL device (Clement Clarke International, UK) at different resistance (R) settings: the high resistance setting (R5) typical of high resistance DPIs, the Low resistance setting (R0) of pMDIs, and the resistance of their current preventer inhaler if different than R0 or R5. Correct (passing) PIFRs were defined as 30–90 L/min for R5 settings and 20–60 L/min for R0 settings. Patients performed up to three inhalations at each setting. If correct PIFR was not generated, two more attempts were given, and simple technique could be taught after every effort.
The results showed that nearly all patients, 93.7% (n=931/994), were able to produce a passing PIFR at the high resistance setting (R5). With the low resistance setting (R0) only 70.5% (n=701/994) managed to inhale at the correct PIFR. All patients who failed with the R0 test inhaled too quickly (>60 L/min).
When patient PIFR was measured with the resistance settings of their current inhaler, one in five (19.8%) patients using a pMDI failed to achieve a PIFR appropriate for low resistance inhalers because they inhaled too fast. This was not the case with the high resistance settings (R5), where only 1.2% (n=4/256) of patients currently using DPIs failed to generate the right PIFR for their inhaler.
Figure 1 displays the PIFRs achieved by patients challenged with low (Figure 1A) and high resistance (Figure 1B) settings, categorized according to their current inhaler resistance level. In the testing of the low resistance setting (R0) the observation was that the higher the resistance in the current inhaler in use, the higher PIFRs the patients tended to generate. Against high resistance (R5) the PIFR results were more homogeneous, regardless of the resistance characteristics of the patient’s current inhaler.
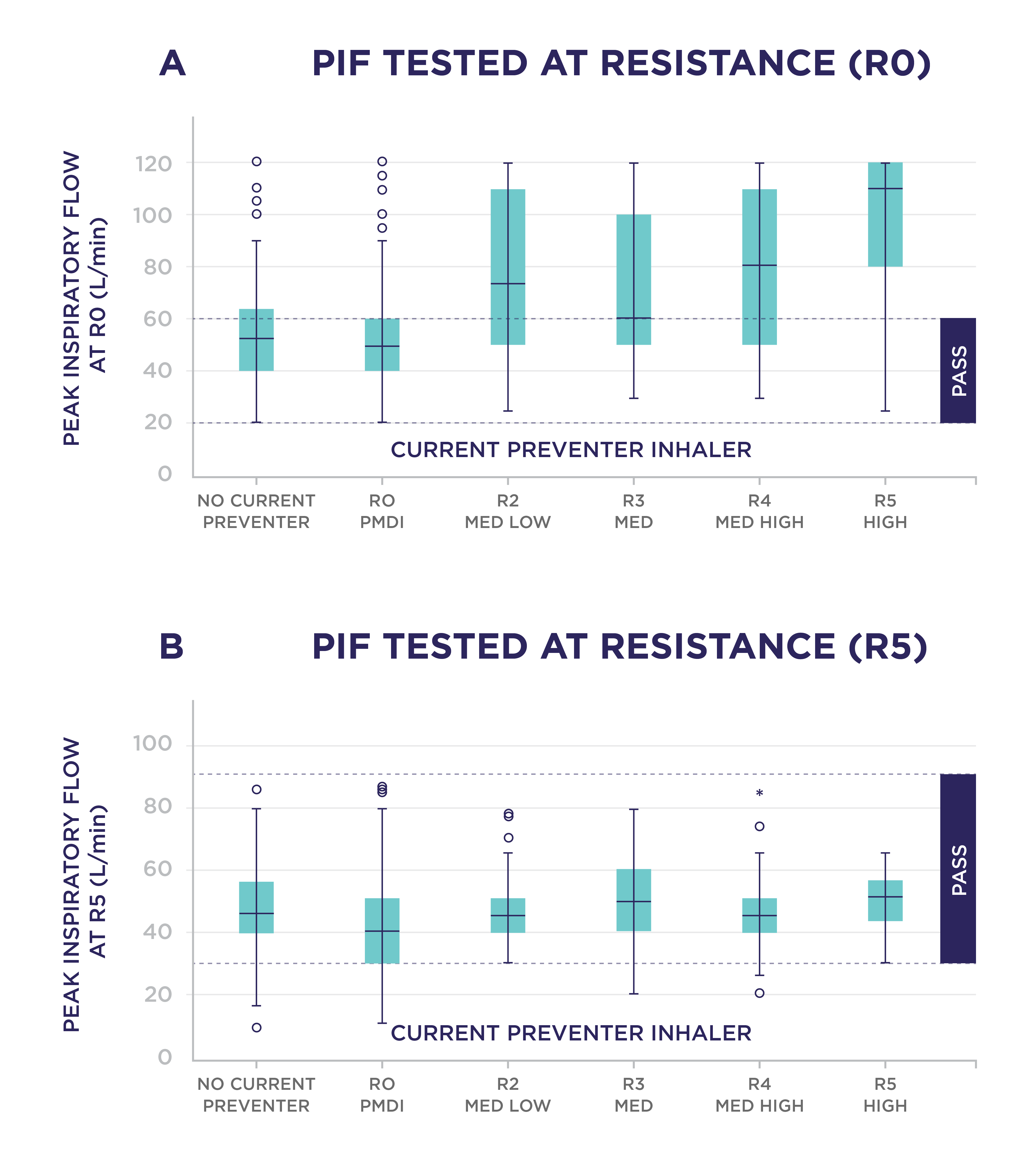
Figure 1. Boxplot of peak inspiratory flow by current preventer resistance at (A) R0 and (B) R5. Horizontal bar of each box indicates median, whereas upper and lower edges of each box represent the upper quartile and lower quartile, respectively. The T-bar extends to 1.5 times the height of the box. An asterisk represents extreme outliers, which are values that are more than 3 times the height of the box. Pass rates for R5 were defined as 30 to 90 L/min and for R0 as 20 to 60 L/min, shown as dashed lines on each figure. Med, Medium. Adapted from Haughney et al 2020.
To summarise, irrespective of their current inhaler and receiving similar training for inhaler technique, the vast majority of patients with asthma were able to generate a PIFR suitable for high-resistance DPIs whereas approximately a third of patients failed to generate a PIFR considered passing for low-resistance pMDIs, due to inhaling too quickly. Even with training nearly 20% of patients currently using a pMDI failed to achieve suitable PIFR for pMDI.
INSTRUCTIONS ON THE USE OF IN-CHECK DIAL G16 (VERSION 2016) WITH EASYHALER® PRODUCTS
Download
Was this article helpful?
Read More:
Reference:
Adverse events should be reported. Reporting forms and information can be found at www.mhra.gov.uk/yellowcard. Adverse events should also be reported to Orion Pharma (UK) Ltd on 01635 520300.
September 2025/RESP-807(1)a(3)



